Exploring Embodied and Bioenergetic Approaches in Trauma Therapy1
Observing Somatic Experience and Olfactory Memory
Sara Invitto & Patrizia Moselli
Bioenergetic Analysis • The Clinical Journal of the IIBA, 2025 (35), 17–36
https://doi.org/10.30820/0743-4804-2025-35-17 CC BY-NC-ND 4.0 www.bioenergetic-analysis.comAbstracts
Recent studies highlight how body psychotherapy is becoming highly cited, especially in connection with studies on trauma-related disorders. This review highlights the theoretical assumptions and recent points in common with embodied simulation and new sensory theories by integrating bioenergetic analysis, embodiment, and olfactory memory in trauma and post-traumatic stress disorder (PTSD) therapy. Embodied memory, rooted in sensorimotor experiences, shapes cognitive functions and emotional responses. Trauma, embodied in somatic experiences, disrupts these processes, leading to symptoms such as chronic pain and dissociation. The literature discussed highlights the impact of burning odors on individuals with PTSD and those who have experienced childhood maltreatment. Burning odors can increase stress and heart rate in war veterans, with sensitivity to these odors intensifying over time since the trauma. Additionally, adults who experienced childhood maltreatment exhibit faster processing of unpleasant odors and increased symptom severity. Grounding techniques, such as adopting a balanced posture, enhance breathing and sensory capabilities, potentially aiding in managing symptoms associated with trauma-related disorders such as PTSD.
Keywords: olfactory memory, post-traumatic stress disorder, bioenergetic analysis, embodied cognition, embodied simulation
Explorando Abordagens Incorporadas e Bioenergéticas na Terapia do Trauma
Observando a Experiência Somática e a Memória Olfativa (Portuguese)
Estudos recentes apontam como a psicoterapia corporal vem se tornando uma referência, bastante relatada – especialmente em estudos sobre desordens relacionadas ao trauma. Está resenha ressalta as afirmações teóricas e aspectos recentes em comum com a simulação corporificada e novas teorias sensoriais através da integração da análise bioenergética, da corporificação e da memória olfativa na terapia do trauma e da Desordem de Stress Pós Traumático (PTSD). A memória corporificada, enraizada em experiências sensório- motoras, formata funções cognitivas e respostas emocionais. O trauma, incorporado através de experiências somáticas, rompe esses processos, levando a sintomas como dores crônicas e dissociação. A literatura destaca o impacto de odores de queimação sobre indivíduos com PTSD, e sobre os que sofreram maus-tratos na infância. Cheiro de queimação aumentaram o stress e causaram aceleração cardíaca em veteranos de guerra, cuja sensibilidade a esses odores aumentaram ao longo do tempo, a partir do trauma. Somando-se a isso, adultos que experimentaram maus-tratos na infância, mostram processamento mais rápido desses odores desagradáveis e recrudescimento severo dos sintomas. Técnicas de grounding, assim como a adoção de posturas de equilíbrio intensificam a respiração e as habilidades sensoriais, auxiliando, potencialmente, no manejo de sintomas associados a desordens relacionados a traumas, como PTSD.
Exploration des approches corporelles et bioénergétiques dans la thérapie du traumatisme
Observation de l’expérience somatique et de la mémoire olfactive (French)
Des études récentes montrent que la psychothérapie corporelle est de plus en plus citée, en particulier en ce qui concerne les études sur les troubles liés aux traumatismes. Cette revue met en évidence des hypothèses théoriques et des points communs récents avec la simulation incarnée et les nouvelles théories sensorielles en intégrant l’analyse bioénergétique, l’embodiment et la mémoire olfactive dans le traitement des traumatismes et du trouble de stress post-traumatique (TSPT). La mémoire incarnée, ancrée dans les expériences sensorimotrices, façonne les fonctions cognitives et les réponses émotionnelles. Le traumatisme, incarné par des expériences somatiques, perturbe ces processus, entraînant des symptômes tels que la douleur chronique et la dissociation. La littérature discutée met en évidence l’impact des odeurs de brûlé sur les personnes atteintes de TSPT et celles qui ont été victimes de maltraitance pendant l’enfance. Les odeurs de brûlé peuvent augmenter le stress et le rythme cardiaque chez les anciens combattants, la sensibilité à ces odeurs s’intensifiant au fil du temps après un traumatisme. De plus, les adultes qui ont été maltraités pendant l’enfance présentent un traitement plus rapide des odeurs désagréables et une sévérité plus forte des symptômes. Les techniques d’ancrage, telles que l’adoption d’une posture équilibrée, améliorent la respiration et les capacités sensorielles, ce qui peut aider à gérer les symptômes associés aux troubles liés aux traumatismes tels que le TSPT.
Esplorazione degli approcci corporei e bioenergetici nella terapia del trauma:
Osservazione dell’esperienza somatica e della memoria olfattiva (Italian)
Recenti studi evidenziano come la psicoterapia corporea stia diventando fortemente citata, specialmente in connessione con gli studi sui disturbi correlati al trauma. Questa relazione evidenzia l’assunzione teorica e i recenti punti emergenti in comune con la simulazione incarnata e le nuove teorie sensoriali integrando ma l’analisi bioenergetica, l’embodiment e la memoria olfattiva nella terapia del trauma e del disturbo post traumatico da stress (PTSD). La memoria embodizzata, che affonda le sue radici nell’esperienza sensomotoria, plasma le funzioni cognitive e le risposte emotive. Il trauma, esperito nelle esperienze somatiche, interrompe questi processi, producendo sintomi come dolore cronico e dissociazione. La letteratura sottolinea l’impatto dell’odore di bruciato su individui con PTSD e coloro che hanno esperito maltrattamenti infantili. Adulti che hanno esperito maltrattamenti infantili manifestano maggiore velocità di elaborazione degli odori spiacevoli e aumento della gravità dei sintomi. Le tecniche di grounding, come l’adottare una postura equilibrata, enfatizzare la respirazione e le capacità sensoriali, sono potenzialmente d’aiuto nella gestione di disturbi correlati al trauma.
Körperorientierte und bioenergetische Ansätze in der Traumatherapie
Die Rolle der somatischen Erfahrung und des Geruchsgedächtnisses (German)
Neuere Studien zeigen, dass die körperorientierte Psychotherapie mehr und mehr erwähnt wird, vor allem in Arbeiten über traumabezogenen Störungen. Unser Bericht unterstreicht die theoretischen Annahmen und Gemeinsamkeiten mit der verkörperten Simulation und den neuen somatischen Theorien, indem er die bioenergetische Analyse, die Verkörperung und das Geruchsgedächtnis in der Traumatherapie und der post-traumatischen Störung (PTSD) integriert. Das in sensomotorischen Erfahrungen verwurzelte verkörperte Gedächtnis formt die kognitiven Funktionen und die emotionalen Reaktionen. Das gleichermaßen in körperlichen Erfahrungen verwurzelte Trauma unterbricht diese Prozesse und führt zu Symptomen wie chronischem Schmerz und Dissoziationen. In der untersuchten Literatur wird der Einfluss von Brandgerüchen auf Personen mit posttraumatischen Störungen und auf Opfer von Kindheitsmisshandlungen hervorgehoben. Brandgerüche können den Stress und die Herzfrequenz bei Kriegsveteranen erhöhen, wobei die Empfindlichkeit gegenüber solchen Gerüchen in der Zeit nach dem Trauma zunimmt. Des Weiteren antworten Erwachsene, die in der Kindheit misshandelt wurden, mit einer schnelleren Reaktion auf schlechte Gerüche und mit einer erhöhten Heftigkeit der Symptome. Die Techniken des grounding, wie z. B. das Einnehmen einer ausgeglichenen Körperhaltung, verbessern die Atmung und die Fähigkeiten der Sinne und helfen potentiell bei der Bewältigung von Symptomen bei traumabezogenen Störungen wie dem PTSD.
Изучение телесного и биоэнергетического подходов в терапии травм
наблюдение за соматическим опытом и обонятельной памятью (Russian)
Недавние исследования показывают, что телесная психотерапия становится все более популярной, особенно в связи с исследованиями расстройств, связанных с травмами. В этом обзоре освещаются теоретические предпосылки и последние моменты, общие для телесного моделирования и новых сенсорных теорий, путем интеграции биоэнергетического анализа, эмбодимента и обонятельной памяти в терапию травм и посттравматических стрессовых расстройств (ПТСР). Телесная память, основанная на сенсомоторном опыте, формирует когнитивные функции и эмоциональные реакции. Травма, проявляющаяся в соматических переживаниях, нарушает эти процессы, что приводит к таким симптомам, как хроническая боль и диссоциация. В обсуждаемой литературе подчеркивается влияние запаха гари на людей с ПТСР и тех, кто в детстве подвергался жестокому обращению. Запах гари может повышать стресс и частоту сердечных сокращений у ветеранов войны, причем чувствительность к этим запахам усиливается с течением времени после травмы. Кроме того, взрослые, которые в детстве подвергались жестокому обращению, быстрее справляются с неприятными запахами и у них усиливается тяжесть симптомов. Техники заземления, такие как принятие сбалансированной позы, улучшают дыхание и сенсорные возможности, потенциально помогая справиться с симптомами, связанными с травмами, такими как ПТСР.
Enfoques corporales y bioenergéticos en la terapia del trauma:
Integración de la experiencia somática y la memoria olfativa (Spanish)
Unos estudios recientes hacen hincapié a que la psicoterapia corporal está siendo muy citada cada vez más, especialmente en relación con estudios sobre trastornos relacionados con el trauma. Este artículo destaca los supuestos teóricos y los puntos recientes en común con la simulación corporizada y las nuevas teorías sensoriales mediante la integración del análisis bioenergético, la corporización y la memoria olfativa en la terapia del trauma y trastorno de estrés postraumático (TEPT). La memoria encarnada, basada en experiencias sensoriomotoras, influye en las funciones cognitivas y las respuestas emocionales, mientras que el trauma, almacenado en el cuerpo, altera estos procesos, generando síntomas como dolor crónico y disociación. La literatura revisada pone de manifiesto el impacto de los olores a quemado en personas con TEPT y en aquellas que han sufrido abusos durante la infancia. Estos olores pueden aumentar el estrés y la frecuencia cardíaca en los veteranos de guerra, y la sensibilidad a los mismos tiende a intensificarse con el paso del tiempo desde el trauma. Además, los adultos que vivieron malos tratos en su infancia procesan más rápidamente los olores desagradables y presentan una mayor severidad de los síntomas. Las técnicas de enraizamiento, como la adopción de una postura equilibrada, mejoran la respiración y las capacidades sensoriales, lo que puede ayudar a controlar los síntomas asociados a trastornos relacionados con el trauma, como el TEPT.
探索创伤治疗中的具身化和生物能量方法
观察躯体体验和嗅觉记忆 (Chinese)
最近的研究表明身心疗法如何变得备受推崇,尤其是与创伤相关疾病的研究。本文通过回顾在创伤和创伤后应激障碍(PTSD)治疗中整合躯体动力分析、具身化和嗅觉记忆,强调了具身化模拟和新感官理论的理论假设和最新共同点。具身记忆植根于感官运动体验,塑造认知功能和情绪反应。具身在躯体体验中的创伤会扰乱这些过程,导致慢性疼痛和解离等症状。讨论的文献强调了燃烧气味对创伤后应激障碍患者和童年遭受虐待者的影响。燃烧的气味会增加退伍军人的压力和心率,创伤后对这些气味的敏感性会随着时间的推移而增强。此外,经历过童年虐待的成年人对难闻气味的反应速度更快,症状的严重程度也会增加。扎根技术,例如采用平衡姿势等可增强呼吸和感知能力,从而可能有助于管理创伤后应激障碍等与创伤相关的症状。
Introduction
Recent studies highlight how body psychotherapy is becoming highly cited, especially in connection with studies on trauma-related disorders. Previously, the literature has not systematized theoretical assumptions and recent points in common with embodied simulation and new sensory theories by integrating bioenergetic analysis, embodied cognition, and olfactory memory in trauma and PTSD therapy. Trauma-related disorders (TRDs) and post-traumatic stress disorders (PTSDs) are expressions in which, by now, a somatic and psychophysiological component has clearly been highlighted. From a psychophysiological point of view, a recent meta-analysis highlighted that the anterior cingulate cortex and the bilateral amygdala are the areas most hyperactivated in PTSD [1]. In contrast, the ventromedial prefrontal cortex and the inferior frontal gyrus appear to be the most inhibited areas. The growth of PTSD involves, as a rule, the shift of the brain state from the high-level processing of multimodal contextual and mnemonic stimuli to primitive formation mediated by the amygdala, of timed sensory associations [2]. The personality differences of each individual (e. g., intelligence, neuroticism, and attention) will influence the stimulus threshold where this change occurs, and consequently affect the subject’s vulnerability [1]. These aspects, connected to an alert system, also profoundly involve the olfactory system, which shares common substrates with emotion, especially fear [3,4]. The theoretical assumptions and recent points are shared with embodied cognition and new sensory theories by integrating bioenergetic analysis, embodied simulation, and olfactory memory in PTSD therapy. Embodied memory, rooted in sensorimotor experiences, shapes cognitive functions and emotional responses. Trauma, embodied in somatic experiences, disrupts these processes, leading to symptoms such as chronic pain and dissociation. Bioenergetic analysis is body psychotherapy developed in the 1950s by Alexander Lowen [5,6] from Reichian assumptions [7]. This analysis focuses on the body’s sensory, perceptual, and cognitive expression, starting from the idea that the unconscious is not a symbolic cerebral representation, even though the unconscious is expressed through the body as a whole. The terms in bioenergetic analysis are linked to “grounding” (i. e., experience) and are strongly connected to the most recent cognitive neuroscience theories on embodied simulation and grounded cognition [8–11]. In addition, the aspects of the grounded experience link it in a very specific way to the theory of integrated information, which sees consciousness as part of a sensory process linked to causality [12–14].
Embodied cognition is an approach that states that mind and body are not distinct, but concur in determining mental and cognitive processes [15]. Gallagher wrote a specific cognitive contribution entitled “How the body shapes the mind”, speaking of “embodied cognition”. In bioenergetic terms, the body shapes the mind, meaning that bodily action in an ecological environment changes our cognition, emotions, and actions. Furthermore, this aspect could be taken to the extreme if we also talk about aspects of epigenetics.
Bodily action can even modify the expression of our phenotypic aspects if we compare these aspects to comparative evolutionary elements. For example, recent studies on environmental (social) handling/enrichment and on neurodegenerative processes in animal models demonstrate how genotypic aspects may not manifest themselves in purely clinical phenotypic aspects [16,17]. This aspect of direct action on the body and with the body seems critical to how body therapy can be read according to different psychophysiological interpretative levels.
The concept of “embodied” begins with W. Reich and A. Lowen, and later in other somatic therapies [18–20]. However, simultaneously, psychophysiology and cognitive neuroscience demonstrated precisely how the body and bodily experience are essential for the development of homeostatic physiological processes and of processes connected to thought and consciousness, as are, in part, the processes described in bioenergetic terms by the bodywork [21,22]. The main concepts of bioenergetics have borrowed the main concepts of embodied theories, albeit in different ways. Grounded cognition and simulation involve the reactivation of perceptual, motor, and introspective states acquired during experience with the world, body, and mind, and offers a unifying vision of cognition [23], emphasizing dynamic brain–body–environment interactions and perception–action links as standard foundations of simple behaviors, as well as of complex cognitive and social skills. Situated cognition is based on the hypothesis that the ecological human–environment interaction can influence individual human development [24,25].
Being “grounded” is also a central aspect of bioenergetic analysis and requires a sense of rootedness that starts from motor/bodily aspects to arrive at emotional and cognitive factors [26]. The meaning of embodied memory arises from a paradigm change that has developed over time, namely the idea that the meaning of symbols is obtained through the sensorimotor experience located in an environmental context. On these premises, many theoretical studies converge on the idea that the body represents how to model higher-level executive functions such as memory.
Starting from these models, the aim of this review would provide a focus on the intersection of bioenergetic analysis, TRD, and PTSD, particularly emphasizing the somatic and psychophysiological components involved. The content explores how trauma affects both the mind and body, leading to symptoms such as chronic pain, dissociation, and altered sensory processing, according to the theoretical underpinnings of embodied simulation and bioenergetic analysis, the first school of thought in body-focused psychotherapy.
Furthermore, the paper delves into the role of embodied memory, highlighting how sensorimotor experiences shape cognitive functions and emotional responses, and how trauma disrupts these processes. It explores the concept of “body muscle memory” and how trauma can lead to muscle tension and various somatic symptoms. The paper also discusses the importance of reconnecting with the body in trauma therapy, emphasizing the role of body psychotherapy in addressing trauma symptoms. Additionally, the paper examines the role of olfactory memory in trauma, emphasizing how smells can trigger traumatic memories and how olfactory stimuli are closely linked to emotional processing. It explores the potential therapeutic implications of incorporating olfactory stimuli into trauma therapy sessions. Overall, the paper aims to provide a comprehensive understanding of how trauma could affect mind–body unity and explore embodied therapeutic approaches in addressing trauma-related disorders (see Figure 1).
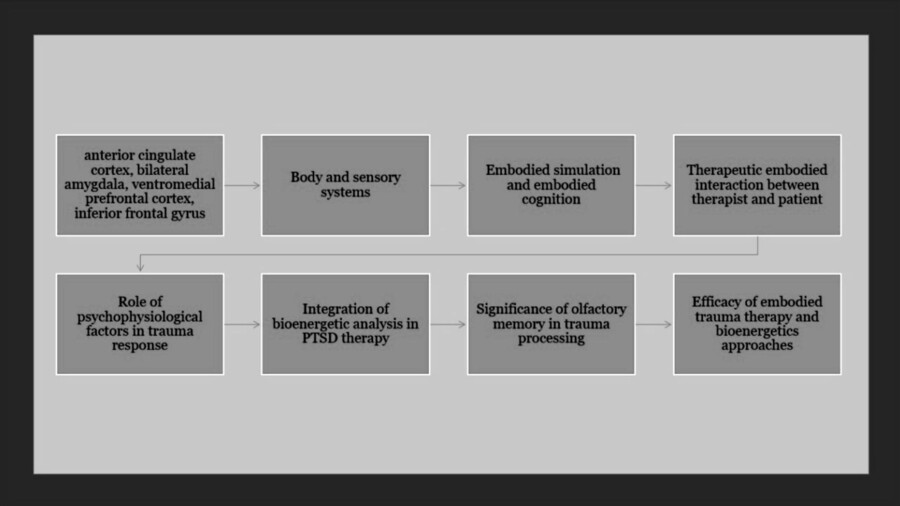
Figure 1. TRS and PTSD in an embodied therapeutic approach through somatic experience and olfactory memory.
Embodied Memory
Common knowledge of embodied memory constitutes those memories thanks to which, for example, action of sitting down or that allow us to orient ourselves easily in spaces of customary use [27–29]. Furthermore, listening to music can viscerally evoke a conversation in the past, and hearing a particular smell can bring to mind an emotional experience [30]. Therefore, sensorimotor reactivation is configured as a constituent of the mnemonic traces through which our cognitive system can retrieve information.
Fuchs stressed that this memory is implicit, that repeated bodily experience is the basis of the process that connects the body to its intention to operate in the environment [31]. In favor of this, Merleau-Ponty expresses the idea of a sensorimotor vision of body memory, capable of providing itself with know-how or the knowledge of how to act with or towards a part of one’s body [15]. Finally, Gallese and Sinigaglia elaborate on a conception of body memory as “a multiplicity of possibilities of action that allows the practical tuning of the body with its environment” [32,33]. Through knowledge of the conceptions that have gradually been endorsed, our experience of the body is not direct, but mediated by perceptual information, influenced by internal information and recalibrated through the implicit and explicit body representation stored, which is body memory. Therefore, it is possible to idealize that memory and, in general, cognitive functions have evolved to serve human action and facilitate interactions between humans and their environment. Thus, cognitive and memory processes are grounded in human experience and intervene in a real-world environment that interferes with perception and involves action. Individual personality is another factor that interferes with our interaction with the environment; according to modern theories, the latter develops through environmental and hereditary factors. Specific to the bodily psychotherapeutic concepts of personality, namely, the bioenergetic model, is the basic idea that life experiences and emotionally significant attitudes manifest physically. Conversely, habitual use of the body affects mental attitudes and basic moods [6]. Consequently, the body should provide relevant information about a person, not only indicating their current emotional state and/or immediate willingness to act, but also about the stable dispositions of thinking, feeling, and behaving. Therefore, according to this perspective, the body is an indispensable component of human existence, and from this point of view, the cognitive and somatic processes evolve in parallel. Another relevant concept is that memories can, to a certain extent, be triggered and brought to consciousness by affective, motor, or sensory stimuli. The experiences of interaction with the environment evoke cognitive and psychosomatic coping strategies or defense [34]. Connection with one’s body has, therefore, played a central role in psychotherapy since its inception: the founders of psychoanalytic therapy considered somatic tensions as an expression of mental conflicts. On the one hand, the body is the stage on which mental disorders develop: in primary care, most patients with psychiatric disorders have somatic symptoms. On the other hand, it is the prerequisite of the psychotherapeutic process in which the patient and therapist communicate verbally and in a bodily dialogue [35,36].
In the case of pathology, Weizsacker’s model of the “Gestaltkreis” explains the invisibility of an individual’s psychological conflict when somatic symptoms replace it [37]. In this sense, psychotherapy strives to find an explanation and a functional solution in which thought, feeling, bodily experience, and expression can be intertwined. For example, “functional relaxation” understands breathing exercises as a semiotic process in which the therapist takes in a client’s bodily signals, interprets them as their own, and verbalizes the result. For this reason, the bioenergetic perspective fits well into the embodied mind paradigm that prevails today in the cognitive sciences. According to this position, human cognition cannot be explained only as a function of the brain, but as an interaction of the entire body and its environment. Shapiro points out that information processing begins in the sensorimotor periphery [38]. From this inevitable evolutionary perspective, human experience and behavior should be understood by their genesis and grounding. Similarly, Petzold and Sieper propose a hermeneutical point of view in which the informed body contains a person’s mental history and state [39].
Recent evidence presents the efficacy of bioenergetic psychotherapeutic treatment in an outpatient setting in Germany and Switzerland, highlighting how, after six months of therapy, the patients showed a significant improvement that tended to be maximized after two years of treatment and was confirmed in follow-up [40]. A systematic review of randomized studies using body psychotherapy in a clinical setting revealed a moderate effect in terms of efficacy on psychopathology and psychological distress [39].
Embodied Trauma and Bioenergetic Therapy
Embodied trauma is represented very well in the conditions of violence suffered. The verbal aspect loses value within a homeostatic process, which instead flows into the somatic system [26,41,42]. This can happen in terms of both awareness and habituation, in posttraumatic stress disorder (PTSD) and also in situations of chronic violence (e. g., domestic violence) [43]. To give meaning to one’s existence, the individual designs, produces, and creates satisfying relationships. Trauma interrupts this process by preventing the individual from staying in the present, so the outside world appears distant, inaccessible, or intrusive. Traumatic experiences, therefore, leave traces in the mind and emotions as well as in the biology and immune system.
The autonomic nervous system, strongly involved in endogenous responses to stress and trauma, is regulated by integrated brainstem reflexes and cranial nerves. It activates the facial, ear, and throat muscles, allowing us to scream, grimace in fear, and listen to incoming help responses [44–46]. If no one responds to the request or the individual does not have the necessary time to ask because the danger is imminent, the body returns to a less relational but more primitive mode of survival, which constitutes the second level: the fight or flight responses (i. e., sympathetic nervous system) [47]. In this, the limbic system comes into play, which activates the sympathetic nervous system by mobilizing the muscles, heart, and lungs to allow for a quick release. If there is no escape, the third level comes into play: freezing or collapsing.
When a person suffers a trauma, they develop somatic symptoms that are a bodily expression of psychological problems; consequently, the body also suffers. This trauma, according to Caizzi, is embodied in the subsymbolic modality that involves the affective, somatic, sensory and motor modalities of mental processing [48]. It is important to note that for many trauma survivors, the body can become a source of pain, intrusion, and shame. Therefore, survivors can often feel disconnected from their bodies. It has been established that exposure to the threat of trauma stimulates the autonomic nervous system, with consequent sympathetic hyper-excitation and parasympathetic hypo-excitation states that accompany survival responses (fight, flight, submission, and freezing). The relevant literature highlights how trauma produces a recalibration of the brain’s alarm system, an increase in stress hormones, and alterations in the system responsible for discriminating irrelevant information. Trauma compromises the area of the brain that transmits the physical, corporeal perception of being alive. These changes account for why traumatized individuals are hypervigilating the threat at the expense of being spontaneously involved in their lives. The human body acts as a “warehouse” for everything an individual experiences during life; this leads to repressed and trapped emotions within multiple parts of the body that cause muscle tension. One of the causes of muscle tension can be precisely trauma: when an individual lives a traumatic experience and does not face it consciously, they are afflicted with fear, a stress that, if chronic, can define the structure of PTSD. All this accumulates within the body, resulting in muscle tension, which contributes to numerous other diseases, such as chronic pain, fibromyalgia, gastrointestinal disorders, and hypertension [49–51]. In this case, we speak of “body muscle memory”, which refers to the traces that the past has imprinted on an individual’s body. There are different types of body memory: memory constituted by the baseline tone of the muscles, which can be altered due to traumatic experiences; memory constituted by habitual postures that represent a limitation in the flexibility of relationships and an unconscious source of malaise and discomfort; memory of movements that, if repeated several times in the same circumstances, become characteristic of a person; and finally, memory of the breath, which, if altered, weighs on the well-being of the subject [52–54]. Therefore, trauma results in a fundamental transformation of how the mind and brain organize perceptions, changing the way we think, our actual ability to think, and our physical and hormonal responses. At the same time, the mind needs to be supported in restructuring the meaning processes associated with trauma; the body needs to learn that the danger has passed and can return to live in the present reality. Therefore, since trauma affects the mind and body, one of the many treatment approaches used is sensorimotor psychotherapy; those who have suffered a trauma lose the “somatic connection” with the present reality: at the body level, the responses are experienced as past events that occur “again and again”; therefore, sensorimotor therapy allows evaluation of and intervention with the trauma symptoms, dealing directly with the body and then accessing the most primitive, automatic, and involuntary brain functions that underlie traumatic and post-traumatic responses [55]. The individual learns to regulate the hyperactivation and physical insensitivity (bodily, cognitive, and emotional experiences) associated with the trauma in a conscious way, being encouraged to observe and carefully describe the interaction between thoughts, emotions, physical sensations, and bodily movements that occur in the here and now. The person can thus discover that the reactions elicited in everyday life are fed by the cognitive patterns linked to the trauma, which activate the defensive responses aimed at survival. It should be noted that memories of trauma are prone to distortion; in fact, most people remember more trauma than they actually experienced. This distortion is due to a failure to monitor their sources: following an experience, intentional and involuntary memories can introduce new details that are assimilated into the person’s memory of the event. To heal from trauma, it would be advisable to start by improving the survivor’s awareness and knowledge of the body’s responses to trauma, with the ultimate goal of localizing a sense of security within the body. This allows the survivor to operate with a deep self-awareness rather than classic conditioning [56].
Trauma victims cannot heal until they become familiar with their bodily sensations. Being scared means having the body always on alert. To change, people need to become aware of their feelings and how the body interacts with the world around it. Body selfawareness is the first step to getting rid of the past. The therapeutic process, therefore, starts primarily from the physical sensations underlying the emotions, such as pressure, heat, muscle tension, tingling, and a sense of emptiness. Observation of bodily changes, such as chest tightness or stomach cramps, when verbalizing negative events from which the person declares not to be disturbed can give space to what is defined as somatic re-enactment or somatic responses to flashbacks related to the unprocessed event. The mind therefore needs to be re-educated to feel physical sensations, and the body needs to be helped to tolerate and enjoy contact well-being. Psychotherapy can therefore act as an intermediary to guide the individual towards a better perception of themself (bodily, emotional, and cognitive) and of the context in which they live. In doing so, psychotherapy will contribute to the psychophysical health of the individual.
Furthermore, healing can be favored by the mirror neuron system, which, due to its plasticity and immediacy, can contribute to new positive experiences that promote the formation of new adaptive, implicit procedural models. This activation can also reside in the prefrontal cortex and is part of a complex neural network that includes afferent and efferent connections to the limbic system, particularly the amygdala and the premotor and motor cortex [57,58]. Recent studies have suggested that MNS-based therapies provide a non-invasive approach to treating emotional disorders because they can modulate them through the mechanism of empathy [58–61].
Olfactory Memory and Bioenergetics: A Model of the Embodied Response Connected to Trauma
Studying the mechanisms of olfactory memory can provide information on the mechanisms of human emotions that can also be applied to the mechanisms of mental disorders involving pathological emotional processing. PTSD is of particular interest because one of its psychobiological mechanisms consists of the failure of the extinction of emotional or traumatic reminders conditioned by fear [45,62].
Olfactory memory is particularly relevant because it is closely linked to intense emotions and is distinguished from other types of memories, such as auditory and visual memory, in that it does not automatically generate verbal and/or visual representations but is, by choice, the most embodied one and evokes affective states and significant episodes. In contrast to the extensive empirical literature on the cognitive processing of verbal and visual memory, few studies have examined the role of smell in emotional or traumatic memories and in trauma-related disorders. The proximal space that the bioenergetic therapist establishes in the session and the use of the body allow, in this case, wider variation and modulation of the olfactory aspect, and also in connection with the gut-brain axis. Within this digression, Gerda Boyesen was one of the first bioenergetic psychoanalysts focused on the interoceptive system and able to use gut–brain feedback [63,64]. An information processing approach commonly includes auditory and visual stimuli to assess perception. Although these involve processes similar to those seen in olfactory memory (processing, encoding, consolidation, and retrieval), olfaction is rarely used to investigate them [65]. This is interesting because it has long been known that adding a salient olfactory cue during learning and retrieval facilitates memory recall [66].
Olfactory Stimuli, Body, and Memory in Trauma
Intrusive re-experiencing, a core symptom of PTSD, has traditionally been described through the mechanism of classical fear conditioning [45,67]. In a study of 100 refugees attending a psychiatric clinic, 45% reported having panic attacks triggered by olfactory stimuli; among these, 58% experienced at least one intrusive memory due to the smell [68]. Patients with PTSD respond intensely to trauma-related danger signals, even in objectively safe environments, and are apparently incapable of adapting their responses based on the contextual signals present. A Vietnam veteran said he was fine until, many years after the war, a Vietnamese restaurant opened near his home: he could not stand the aroma of a typical sauce used to season fish, which he had smelled several times in Vietnam. The former soldier stated that the smell brought back memories of his war experiences, making him feel discomfort and the strange sensation of being torn and covered in blood [69]. Some studies have also demonstrated increased odor detection and sympathetic arousal, including skin conductance and heart rate, in correspondence with odors related to fear, trait anxiety, or mood disorder anxiety [70]. Smells can trigger ancient and emotional memories, including memories of traumatic experiences, because the anatomy of the olfactory system involves activation of the same brain structures that support emotion processing (limbic system and medial temporal lobe circuits) and declarative memory [71].
To understand the cerebral processes involved in PTSD, it is also important to study the functioning of the breath and the olfactory system. Some studies in the literature have examined the effect of burning odors on war veterans, and it has been demonstrated that heart rate increases as a function of the negative valence (i. e., the unpleasantness), causing an increase in the stress and anguish suffered by soldiers with PTSD [72]. Sensitivity to burning odors is also correlated with the time that has passed since the trauma: in contrast to the general symptoms of PTSD, which tend to become less severe as time passes, the symptoms triggered by these types of odors can intensify [73]. Additionally, a study conducted by Croy and colleagues measured odor-related chemosensory potentials in adults who had experienced childhood maltreatment, reporting a faster processing of unpleasant odors and the increased severity of symptoms of the disorder. Grounding – positioning the subject in a posture in which they should be balanced – allows and amplifies the possibility of breathing [74]. In turn, breathing enables an increase in attentional and sensory capabilities, both physical and chemoreceptive, and also enhances aspects connected to interoception and memory retrieval [71,75].
Conclusions
This review explores the intersection of TRD, PTSD, and body psychotherapy, mainly focusing on the concept of embodied simulation and its implications for therapeutic intervention in bioenergetic psychotherapy. It emphasizes that trauma affects both the mind and body, necessitating integrated and embodied therapeutic interventions. The concept of embodied memory, rooted in sensorimotor experiences, is highlighted as a critical aspect of understanding how trauma affects cognitive functions and emotional responses. Recognizing the role of bodily sensations and reactions is crucial in addressing trauma-related symptoms. The efficacy of bioenergetic psychotherapeutic treatment in addressing TRS suggests significant improvements in psychopathology and psychological distress over time. Moreover, the paper discusses the significance of olfactory memory in trauma processing and symptomatology. It suggests that olfactory stimuli can trigger emotional memories, emphasizing the need to incorporate olfactory experiences into therapeutic interventions. These aspects have practical implications for clinical practice, including incorporating somatic interventions, breathwork, and sensory experiences into trauma therapy sessions.
We also emphasize the need for therapists to be attuned to clients’ verbal and nonverbal cues, including bodily sensations and emotional responses.
Future research could focus on exploring the neural mechanisms underlying embodied memory, investigating the specific effects of olfactory stimuli on trauma processing, and further evaluating the long-term effectiveness of bioenergetic therapy for trauma-related disorders.
Furthermore, this review highlights the importance of adopting an integrated, embodied approach to trauma therapy, incorporating insights from clinical psychology, cognitive neuroscience, psychophysiology, and bioenergetic practice.
Acknowledgments
The authors acknowledge G. Piraino, R. D. Greco, and G. Gatto for supporting the introductive bibliography; M. R. Filoni and L. Agresti for supporting the paper; and V. Heinrich-Clauer for her fondness and appreciation.
Annotation
- [1]
- This text is a reprint of: Invitto, S. & Moselli, P. (2024). Exploring Embodied and Bioenergetic Approaches in Trauma Therapy: Observing Somatic Experience and Olfactory Memory. Brain Sciences, 14(4), 385. https://doi.org/10.3390/brainsci14040385
References
1. Pitman, R. K., Rasmusson, A. M., Koenen, K. C., Shin, L. M., Orr, S. P., Gilbertson, M. W., Milad, M. R. & Liberzon, I. (2012). Biological Studies of Post-Traumatic Stress Disorder. Nat. Rev. Neurosci., 13, 769–787.
2. Phelps, E. A. & LeDoux, J. E. (2005). Contributions of the Amygdala to Emotion Processing: From Animal Models to Human Behavior. Neuron, 48, 175–187.
3. Canteras, N. S., Pavesi, E. & Carobrez, A. P. (2015). Olfactory Instruction for Fear: Neural System Analysis. Front. Neurosci., 9, 276.
4. Soudry, Y., Lemogne, C., Malinvaud, D., Consoli, S. M. & Bonfils, P. (2011). Olfactory System and Emotion: Common Substrates. Eur. Ann. Otorhinolaryngol. Head. Neck Dis., 128, 18–23.
5. Cockburn, G. (2013). “Seeing What Is so Simply Present”. Clin. J. Int. Inst. Bioenerg. Anal., 23, 75–99.
6. Guest, D., Parker, J. & Williams, S. L. (2019). Development of Modern Bioenergetic Analysis. Body Mov. Danc. Psychother., 14, 264–276.
7. Hall, J. (2015). Roots and History of Humanistic Psychology. Self Soc., 43, 69–75.
8. Wilson, M. (2002). Six Views of Embodied Cognition. Psychon. Bull. Rev., 9, 625–636.
9. Varela, F. J., Thompson, E., Rosch, E. & Kabat-Zinn, J. (2016). The Embodied Mind: Cognitive Science and Human Experience. Cambridge, MA: Mit Pr.
10. Gallese, V. (2016). Finding the Body in the Brain: From Simulation Theory to Embodied Simulation. In H. Kornblith & B. McLaughlin (Eds.), Goldman and his Critics (pp. 297–317). Malden, MA: Blackwell.
11. Gallese, V. & Sinigaglia, C. (2011). What Is so Special about Embodied Simulation? Trends Cogn. Sci., 15, 512–519.
12. Tononi, G. (2008). Consciousness as Integrated Information: A Provisional Manifesto. Biol. Bull., 215, 216–242.
13. Bucci A. & Grasso M. (2017). Sleep and Dreaming in the Predictive Processing Framework. In T. Metzinger & W. Wiese (Eds.), Philosophy and Predictive Processing: 6. Frankfurt am Main: MIND Group. https://doi.org/10.15502/9783958573079
14. Marzola, G., Di Carlo, P. & Brancucci, A. (2019). The Relativity of Consciousness: The Application of Time Dilation to the Theory of Integrated Information. NeuroQuantology, 17, 45–57.
15. Gallagher, S. (2010). Merleau-Ponty’s Phenomenology of Perception. Topoi, 29, 183–185.
16. Fernández-Teruel, A., Giménez-Llort, L., Escorihuela, R. M., Gil, L., Aguilar, R., Steimer, T. & Tobea, A. (2002). Early-Life Handling Stimulation and Environmental Enrichment: Are Some of Their Effects Mediated by Similar Neural Mechanisms? Pharmacol. Biochem. Behav., 73, 233–245.
17. Muntsant-Soria, A. & Gimenez-Llort, L. (2020). Impact of Social Isolation on the Behavioral and Functional Profiles and Hippocampal Atrophy Asymmetry in Dementia in Times of Coronavirus Pandemic (COVID-19): A Translational Neuroscience Approach. Front. Psychiatry, 11, 1126.
18. Sletvold, J. (2011). “The Reading of Emotional Expression”: Wilhelm Reich and the History of Embodied Analysis. Psychoanal. Dialogues, 21, 453–467.
19. Sletvold, J. (2014). The Embodied Analyst: From Freud and Reich to Relationality. London: Routledge.
20. Glazer, R. & Friedman, H. (2010). Re-Embodying the Mind and Re-Minding the Body: In Memoriam to Alexander Lowen. Humanist. Psychol., 38, 196–198.
21. Hilton, R. (2012). The Ever Changing Constancy of Body Psychotherapy. Int. Body Psychother. J. Art. Sci. Somat. Prax., 11, 74–93.
22. Sabin-Farrell, R. & Bretherton, R. (2016). Body-Centred Psychotherapy (BCP). In D. Dawson & N. Moghaddam (Eds.), Formulation in Action (pp. 142–160). Warsaw: De Gruyter Open.
23. Barsalou, L. W. (2010). Grounded Cognition: Past, Present, and Future. Top. Cogn. Sci., 2, 716–724.
24. Clancey, W. J. (1997). Situated Cognition: On Human Knowledge and Computer Representations. Cambridge, UK: Cambridge University Press.
25. Rencic, J., Schuwirth, L. W. T., Gruppen, L. D. & Durning, S. J. (2020). A Situated Cognition Model for Clinical Reasoning Performance Assessment: A Narrative Review. Diagnosis, 7, 227–240.
26. Bartanian, G. J. (2019). Mindful Grounding and Trauma. Rosemead, CA: University of the West.
27. Arminjon, M., Preissmann, D., Chmetz, F., Duraku, A., Ansermet, F. & Magistretti, P. J. (2015). Embodied Memory: Unconscious Smiling Modulates Emotional Evaluation of Episodic Memories. Front. Psychol., 6, 650.
28. Ian., F. (2019). Embodied Memories: Reviewing the Role of the Body in Memory Processes. Psychon. Bull. Rev., 26, 1747–1766.
29. Marre, Q., Huet, N. & Labeye, E. (2021). Embodied Mental Imagery Improves Memory. Q. J. Exp. Psychol., 74, 1396–1405.
30. Invitto, S. & Grasso, A. (2019). Chemosensory Perception: A Review on Electrophysiological Methods in “Cognitive Neuro-Olfactometry”. Chemosensors, 7, 45.
31. Fuchs, T. (2012). The Phenomenology of Body Memory. In S. C. Koch, T. Fuchs, M. Summa & C. Muller (Eds.), Body Memory, Metaphor and Movement (pp. 84–89). Amsterdam: John Benjamins.
32. Gallese, V. & Sinigaglia, C. (2010). The Bodily Self as Power for Action. Neuropsychologia, 48, 746–755.
33. De Bruin, L. & Gallagher, S. (2012). Embodied Simulation, an Unproductive Explanation: Comment on Gallese and Sinigaglia. Trends Cogn. Sci., 16, 98–99.
34. Sollmann, U. (2011). Treatment of Psychosomatic Disorders in Bioenergetic Analysis. In V. Heinrich-Clauer (Ed.), Handbook Bioenergetic Analysis (pp. 363–368). Giessen: Psychosozial-Verlag.
35. Heinrich-Clauer, V. (2011). Handbook Bioenergetic Analysis. Giessen: Psychosozial-Verlag.
36. Kuhntopp, J. & Heinrich, V. (2001). Bioenergetic Duos – Uncovering Deficits in Mother-Child Relationships. In C. D. Ventling (Ed.), Childhood Psychotherapy: A Bioenergetic Approach (pp. 23–31). Berlin: S. Karger.
37. Frangi, S. (2012). Weizsacker et Les Autres: Merleau-Ponty Lettore Del Gestaltkreis. Chiasmi Int., 14, 161–193.
38. Shapiro, L. (2019). Embodied Cognition. London: Routledge.
39. Rosendahl, S., Sattel, H. & Lahmann, C. (2021). Effectiveness of Body Psychotherapy. A Systematic Review and Meta-Analysis. Front. Psychiatry, 12, 709798.
40. Komeda-Lutz, M. (2006). Is There Healing Power in Rage?: The relative contribution of cognition, affect and movement to psychotherapeutic processes. Clin. J. Int. Inst. Bioenerg. Anal., 16, 103–127.
41. Culbertson, R. (1995). Embodied Memory, Transcendence, and Telling: Recounting Trauma, Re-Establishing the Self. New Lit. Hist., 26, 169–195.
42. O’Brien, C. V. & Charura, D. (2022). Refugees, Asylum Seekers, and Practitioners’ Perspectives of Embodied Trauma: A Comprehensive Scoping Review. Psychol. Trauma, online ahead of print.
43. Invitto, S., Mignozzi, A., Piraino, G., Rocco, G., De Feudis, I., Brunetti, A. & Bevilacqua, V. (2017). Artificial Neural Network Analysis and ERP in Intimate Partner Violence. Multidiscip. Approaches Neural Comput., 69, 247–257.
44. Trachtman, J. N. (2010). Post-Traumatic Stress Disorder and Vision. Optometry, 81, 240–252.
45. Vermetten, E. & Lanius, R. A. (2012). Biological and Clinical Framework for Posttraumatic Stress Disorder. Handb. Clin. Neurol., 106, 291–342.
46. Biltz, R. G., Sawicki, C. M., Sheridan, J. F. & Godbout, J. P. (2022). The Neuroimmunology of Social-Stress-Induced Sensitization. Nat. Immunol., 23, 1527–1535.
47. Sherin, J. E. & Nemeroff, C. B. (2011). Post-Traumatic Stress Disorder: The Neurobiological Impact of Psychological Trauma. Dialogues Clin. Neurosci., 13, 263–278.
48. Caizzi, C. (2012). Embodied Trauma: Using the Subsymbolic Mode to Access and Change Script Protocol in Traumatized Adults. Trans. Anal. J., 42, 165–175.
49. Fisher, E., Law, E., Dudeney, J., Palermo, T. M., Stewart, G. & Eccleston, C. (2018). Psychological Therapies for the Management of Chronic and Recurrent Pain in Children and Adolescents. Cochrane Database Syst. Rev., 9, CD003968.
50. Nadal-Nicolás, Y., Rubio-Arias, J.Á., Martínez-Olcina, M., Reche-García, C., Hernández-García, M. & Martínez-Rodríguez, (2020). A. Effects of Manual Therapy on Fatigue, Pain, and Psychological Aspects in Women with Fibromyalgia. Int. J. Environ. Res. Public Health, 17, 4611.
51. Delussi, M., Piraino, G., Guerzoni, S., Castro, F. L., Sances, G., Guaschino, E., Vaghi, G., Grazzi, L., Sacco, S., Onofri, A. et al. (2023). Gender-Related Stress Factors and Emotional Perception in Migraine: A Structured Online Questionnaire in Migraine Patients and Controls. Neurol. Sci., 45, 1645–1654.
52. Grassmann, M., Vlemincx, E., von Leupoldt, A., Mittelstadt, J. M. & Van den Bergh, O. (2016). Respiratory Changes in Response to Cognitive Load: A Systematic Review. Neural Plast., 2016, 8146809.
53. Fincham, G. W., Strauss, C. & Cavanagh, K. (2023). Effect of Coherent Breathing on Mental Health and Wellbeing: A Randomised Placebo-Controlled Trial. Sci. Rep., 13, 22141.
54. Maric, V., Ramanathan, D. & Mishra, J. (2020). Respiratory Regulation & Interactions with Neuro-Cognitive Circuitry. Neurosci. Biobehav. Rev., 112, 95–106.
55. Ogden, P., Pain, C. & Fisher, J. (2006). A Sensorimotor Approach to the Treatment of Trauma and Dissociation. Psychiatr. Clin. N. Am., 29, 263–279.
56. O’Shea Brown, G. (2021). Healing Complex Posttraumatic Stress Disorder: A Clinician’s Guide. Berlin/Heidelberg: Springer.
57. Prof, B. & Hurley, S. (2007). The Shared Circuits Model: How Control, Mirroring and Simulation Can Enable Imitation, Deliberation, and Mindreading. Behav. Brain Sci., 31, 1–22.
58. Hausser, L. F. (2012). Empathy and mirror neurons. A view on contemporary neuropsychological empathy research. Prax. Kinderpsychol. Kinderpsychiatr., 61, 322–335.
59. Khalil, R., Tindle, R., Boraud, T., Moustafa, A. A. & Karim, A. A. (2018). Social Decision Making in Autism: On the Impact of Mirror Neurons, Motor Control, and Imitative Behaviors. CNS Neurosci. Ther., 24, 669–676.
60. Sosic-Vasic, Z., Eberhardt, J., Bosch, J. E., Dommes, L., Labek, K., Buchheim, A. & Viviani, R. (2019). Mirror Neuron Activations in Encoding of Psychic Pain in Borderline Personality Disorder. Neuroimage Clin., 22, 101737.
61. Van Overwalle, F. & Baetens, K. (2009). Understanding Others’ Actions and Goals by Mirror and Mentalizing Systems: A Meta-Analysis. NeuroImage, 48, 564–584.
62. Yehuda, R., Hoge, C. W., McFarlane, A. C., Vermetten, E., Lanius, R. A., Nievergelt, C. M., Hobfoll, S. E., Koenen, K. C., Neylan, T. C. & Hyman, S. E. (2015). Post-Traumatic Stress Disorder. Nat. Rev. Dis. Primers, 1, 1–22.
63. Boyesen, G. (1999). Tra Psiche e Soma: Introduzione Alla Psicologia Biodinamica. General Santos City: Astrolabio.
64. Westland, G. (2006). Personal Reflections on Gerda Boyesen 1922–2005. Body Mov. Danc. Psychother., 1, 155–160.
65. Koster, E. P. (2005). Does Olfactory Memory Depend on Remembering Odors? Chem. Senses, 30, i236–i237.
66. Morgan, C. D. & Murphy, C. (2010). Differential Effects of Active Attention and Age on Event-Related Potentials to Visual and Olfactory Stimuli. Int. J. Psychophysiol., 78, 190–199.
67. Shin, L. M., Kosslyn, S. M., McNally, R. J., Alpert, N. M., Thompson, W. L., Rauch, S. L., Macklin, M. L. & Pitman, R. K. (1997). Visual Imagery and Perception in Posttraumatic Stress Disorder: A Positron Emission Tomographic Investigation. Arch. Gen. Psychiatry, 54, 233–241.
68. Hinton, D. E., Pham, T., Tran, M., Safren, S. A., Otto, M. W. & Pollack, M. H. (2004). CBT for Vietnamese Refugees with Treatment-Resistant PTSD and Panic Attacks: A Pilot Study. J. Trauma. Stress., 17, 429–433.
69. Daniels, J. K. & Vermetten, E. (2016). Odor-Induced Recall of Emotional Memories in PTSD – Review and New Paradigm for Research. Exp. Neurol., 284, 168–180.
70. Lombion-Pouthier, S., Vandel, P., Nezelof, S., Haffen, E. & Millot, J.-L. (2006). Odor Perception in Patients with Mood Disorders. J. Affect. Disord., 90, 187–191.
71. Larsson, D. E. O., Esposito, G., Critchley, H. D., Dienes, Z. & Garfinkel, S. N. (2021). Sensitivity to Changes in Rate of Heartbeats as a Measure of Interoceptive Ability. J. Neurophysiol., 126, 1799–1813.
72. Cortese, B. M., Uhde, T. W., Larowe, S. D., Stein, S. V., Freeman, W. C., McClernon, F. J., Brady, K. T. & Hartwell, K. J. (2015). Olfactory Cue Reactivity in Nicotine-Dependent Adult Smokers. Psychol. Addict. Behav., 29, 91–96.
73. Perkonigg, A., Pfister, H., Stein, M. B., Hofler, M., Lieb, R., Maercker, A. & Wittchen, H.-U. (2005). Longitudinal Course of Posttraumatic Stress Disorder and Posttraumatic Stress Disorder Symptoms in a Community Sample of Adolescents and Young Adults. AJP, 162, 1320–1327.
74. Zeren, M., Cakir, E. & Gurses, H. N. (2019). Effects of Inspiratory Muscle Training on Postural Stability, Pulmonary Function and Functional Capacity in Children with Cystic Fibrosis: A Randomised Controlled Trial. Respir. Med., 148, 24–30.
75. Molle, L. & Coste, A. (2022). The Respiratory Modulation of Interoception. J. Neurophysiol., 127, 896–899.
About the Authors
Sara Invitto, PhD, SIAB and IIBA Psychologist and Psychotherapist, is Associate Professor of General Psychology S. S. D. PSIC-01/A, qualified as Full Professor in the competitive sector. She is the scientific representative of the INSPIRE Laboratory, a laboratory on the Cognitive and Psychophysiological Olfactory Processes (Department of Biological and Environmental Sciences and Technologies, University of Salento). She deals with clinical processes (e. g., anosmia) and basic processes connected to olfactory perception and the study of higher cognitive functions. Within the research topic connected to smell, she has established scientific collaborations with companies and with national and international academic structures, both in clinical research and in the field of new technologies; furthermore, she is the author of numerous publications in the field of cognitive neuroscience.
Patrizia Moselli, Psychologist, psychotherapist, International Trainer, Member of the Faculty and Board of Trustees of IIBA, President of the Italian Society of Bioenergetic Analysis (SIAB), Past President of FIAP (Italian Federation of of Psychotherapy Associations) member of the Board of Directors of SIPSIC (Italian Society of Psychotherapy).